Sleep-disordered breathing is a spectrum of disorders involving breathing alterations during sleep. At one end is snoring – a disorder considered to be a purely cosmetic complaint without identified health implications. Tissue in the throat simply vibrates. At the other end is obstructive sleep apnea, otherwise known as OSA. In OSA, there is snoring, but also enough tissue obstruction to lower airflow. This leads to decreased oxygen levels and frequent awakenings, disturbances which translate into serious health implications.
Obstructive Sleep Apnea (OSA)
OSA is thought to affect 3-4% of the adult population and as much as 5-10% of the pediatric population. Poor sleep quality in adults leads to concentration problems, memory loss, daytime sleepiness, and morning headaches. In children, OSA leads to decreased intelligence, decreased executive functioning, bedwetting, hyperactivity, and attention disorders. OSA is linked to diabetes, coronary artery disease, hypertension, and stroke. In children, it is also linked to heart failure and stunted growth.
So how do we identify OSA? Adults require a sleep study to measure multiple parameters during sleep to make the diagnosis. This study can be performed at home in most cases. In the majority of children, mom and dad serve as the sleep study. I ask them to identify long pauses in breathing and gasping during sleep to make the diagnosis. If there is ever any doubt, a sleep study is also an option.
OSA Treatment
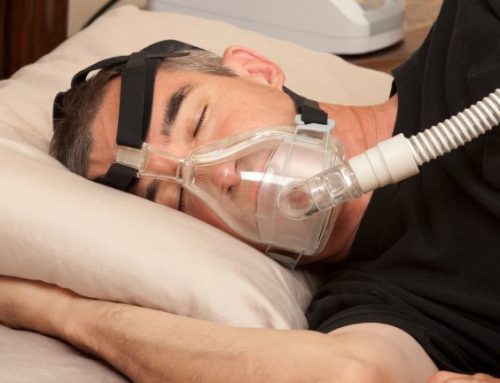
If sleep apnea is diagnosed, treatment must be initiated. In adults, first-line therapy is a continuous positive airway pressure (CPAP) device. Most people have difficulty tolerating these devices. If you are a patient who cannot tolerate CPAP, other therapies include mandibular splints or surgery. If surgery is the chosen option, it is critical to identify the areas of obstruction in the nose and throat causing OSA. Some patients need nasal surgery (e.g., septoplasty, turbinate reduction, polyp removal). Others need their tonsils removed and soft palate trimmed. Still others will need their lower throats treated with a technique call a tongue base reduction. This is usually done with a laser attached to a microscope or with an exciting new technique called transoral robotic surgery (TORS). One of our specialists, Dr. Nason, is one of very few surgeons in the US performing TORS to address sleep apnea by reducing the tongue base in properly selected patients.
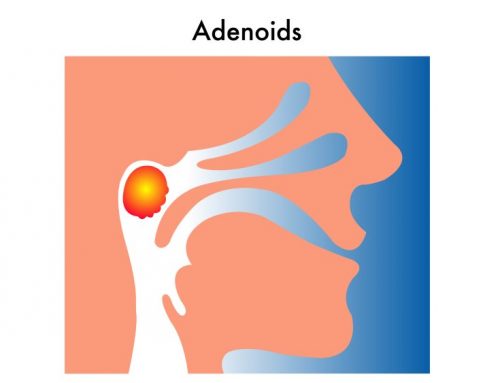
The first line treatment for OSA in children is tonsillectomy and adenoidectomy. This simple surgery boasts a success rate as high as 85%. If sleep apnea persists despite having tonsillectomy and adenoidectomy, we can utilize a new technique called drug-induced sleep endoscopy to identify the specific site of obstruction that should next be addressed.
The bottom line is that OSA should always be addressed in both children and adults. The health consequences are far too important to ignore the possibility of OSA in yourself or a loved one. If you have any concern about the presence of OSA or an ENT related issue, please feel free to come in for a consultation.



Leave A Comment